The information provided in this article does not replace your relationship with your personal family physician or eye care specialist. It should be used as a general guide only, and not as the ultimate source of information on eye health.
At 37, I was too busy with work and home life to research non-invasive treatment options for heavy menstruation, a monthly painful inconvenience I was afflicted with since I was 11-years-old. Instead, I signed up for the first and most aggressive solution presented to me: the surgical removal of my healthy reproductive organs.
Rather than forewarn me about the many risks with the surgery, and its potentially negative impacts, my then family physician said I should consider myself lucky to be able to avoid cancer of the ovaries, uterus, fallopian tubes, and cervix. The gynecologist, however, did say I wouldn’t be able to live without estrogen replacement therapy (ERT) once my ovaries were excised, and that he would provide me with a prescription before my discharge from the hospital.
At the time, I was a compliant patient who wouldn’t have dared to question a medical expert’s opinion and judgement. As a result, I was uninformed about the risks and side effects associated with ERT, and the consequences that the loss of my ovaries would have for my overall hormonal well-being.
The possible link between hormonal and eye health
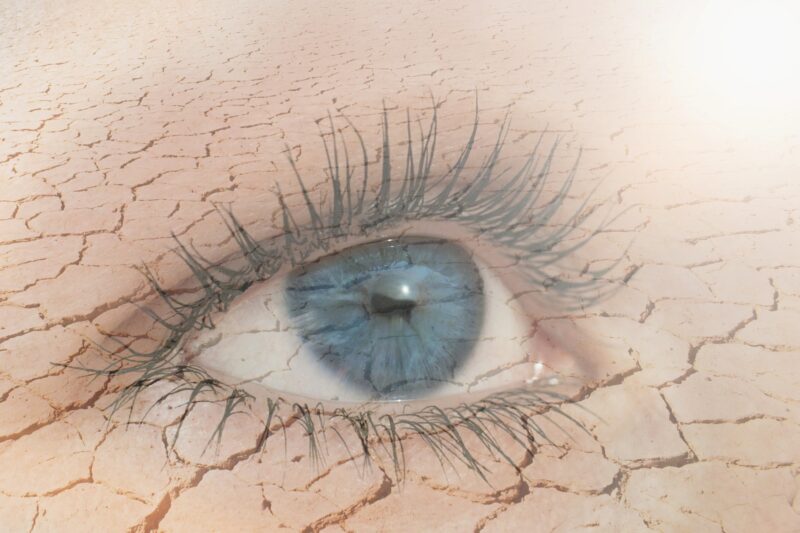
A recent study conducted by the American non-profit Society for Women’s Health Research (SWHR) concluded that 61% of perimenopausal and menopausal women suffer from evaporative dry eye, a condition that can result in light sensitivity and blurred vision. The Society’s surveys suggest that this group of women may be unaware of the link between hormonal fluctuations and dry eye, and that most seek relief from over-the-counter eye drops instead of speaking to their doctor about it.
My vision was seriously affected by dry eye, and sensitivity to light, long before I started to experience the life-changing symptoms of surgical menopause – and I talked about it to any eye specialist willing to listen. Could it be that I was hormonally unbalanced for most of my life? Somehow, I have my doubts about that. I believe my hectic lifestyle and poor eating habits likely played as significant a role in all aspects of my health, including the dry eye issue. Thankfully, I came to my senses about eating more healthily once I reached my 40’s.
I started to wear prescription glasses at age 7, and by the time I underwent cataract surgery at 72, I was wearing glasses that looked like a magnifying glass. But, at annual appointments with optometrists, and occasional referrals to ophthalmologists once my problem with dry eye became more difficult to endure, there was never any mention of the effect my hormonal health could have on my vision. It’s not an issue I would have brought up on my own either. Not with an eye specialist, anyway. Besides, regular blood tests over the years never indicated any significant hormonal abnormalities.
In my situation, perhaps the link between hormonal and eye health can be made because my problem with dry eye caused sleep disorders and insomnia that impacted my quality of life as greatly as the hot flashes and night sweats related to surgical menopause.
The cataract surgery effect
While cataract surgery is generally safe and effective, there are some risks and side effects. These include blurry and unclear vision and, lo and behold, dry eye! The dry eye side effect can be linked to the small number of nerves on the surface of the eye that get cut when the surgeon makes the necessary incisions to reach a foggy lens. Other aftereffects include light sensitivity, arc of light or crescent-shaped shadow in the post-surgery visual field, red eye normally caused by inflammation, floaters, and droopy or twitching eyelids. It’s a lot of information to consider, but an important step nonetheless, to make an informed decision about the procedure before undergoing the surgery.
In menopausal and post-menopausal women with pre-existing conditions of dry eye and sensitivity to light, an aggravation of symptoms is inevitable once the foggy lenses are removed and replaced with clear lenses. It’s what happened to me. I can’t tolerate sunlight, working from screens has to be limited, and street lighting and bright headlights on vehicles prevent me from driving at night.
Dry eye treatment options
According to the Mayo Clinic, dry eye disease (DED) occurs when eyes no longer produce enough tears. If the limited tears produced evaporate too quickly, the insufficient lubrication leads to inflammation, discomfort, burning, stinging, and redness, all symptoms resulting in lower quality of life if treatments can’t provide relief.
For those interested in the more technical definition for DED, it has recently been updated by The Tear Film and Ocular Surface Society (TFOSS) at its Dry Eye Workshop (DEWS) III: ‘Dry eye is a multifactorial, symptomatic disease characterized by a loss of homeostasis of the tear film and/or ocular surface, in which tear film instability and hyperosmolarity, ocular surface inflammation and damage, and neurosensory abnormalities are etiological factors.’
Fortunately, there are several treatment options available. Depending on the severity of the condition, preservative-free eye drops, warm compresses for 10-minutes daily, using a specialized heat mask to help open oil glands, increasing omega-3 intake, and use of humidifiers can provide effective non-drug alternatives to alleviate pain.
As well, there are new diagnostic and therapeutic approaches. For example, Intense Pulse Light (IPL) therapy is an in-office non-invasive procedure using light pulses to treat DED by targeting the inflammation and melting the clogged oils in eyelid glands. IPL can improve tear film stability between blinks to prevent rapid evaporation and dryness.
Although there have been recent reports and articles from various medical sources suggesting that ERT might be a treatment option for dry eye, both the Journal of the American Medical Association (JAMA), and the U.S. National Institutes of Health published data in 2001 suggesting that perimenopausal and menopausal women who use hormone replacement therapies (HRT), particularly estrogen alone, are actually putting themselves at increased risk for DED.
In 2019, a similar important study was published in the Canadian Journal of Ophthalmology (CJO). The focus of that study was to review data from previous studies to determine the correlation between HRT/ERT and DED. It concluded that while hormone replacement therapies might be helpful in relieving menopausal symptoms in some women, they did not reliably provide relief for dry eye disease.
Whether for relief of dry eye or menopausal symptoms, the decision to take any form of hormonal replacement therapy is a personal one. The risks are different for everyone, and they can be influenced by health history, dosage, type, and duration of treatment. The Canadian Cancer Society recommends talking to a healthcare provider for the best advice on HRT’s associated health risks such as increased risk of breast cancer, blood clots, stroke, and heart disease.
Nowadays, there are other medications for dry eye to help preserve natural tears without having to use products that could result in new issues, or an exacerbation of the symptoms from which menopausal women with DED are trying to get relief. Based on my experience, Hylo eye drops provide the longest lasting relief of all the over-the-counter drops I’ve tried. This Canadian product is preservative-free, and safe to use for as many years as needed. It can be purchased from eye clinics, and it is also available on amazon.ca.
The proactive approach
Regular exams with an ophthalmologist, or a doctor of optometry, are especially important for eye health during menopause. Dry eye and sensitivity to light can be life-changing events, but if you have a specialist willing to go the extra mile with solutions, good eye health can be maintained throughout the menopausal and post-menopausal years.
The best advice is to take early action against dry eye syndrome before it leads to serious corneal damage and vision issues. Managing the condition in its early stages, with lifestyle changes and consistent care, can prevent symptoms from becoming more serious.
Despite my challenges with dry eye and sensitivity to light, I am grateful for my sight, and I plan to continue to do all that I can to hang on to it. I don’t consider it a problem to live out the rest of my life in soft lighting only. It makes for a most relaxing home environment, actually. Of course, my anti-inflammatory diet, the application of drops throughout the day and night, tinted glasses, and warm compresses in the evening are essential to my daily routine, and all provide a reduction of discomfort and distress.
Karen Carpenter may have sung about rainy days bringing her down, but for me, the opposite is true. I find rainy and muggy days to be of great soothing benefit to my dry eyes. Maybe I should consider moving to Prince Rupert, B.C., Canada’s wettest city!
Lise Cloutier-Steele is an Ottawa writer, the author of Misinformed Consent: Women’s Stories about Unnecessary Hysterectomy, available from www.amazon.com (U.S. edition only), and the 2025 Edition of There’s No Place Like Home: A guide to help caregivers manage the long-term care experience, available from www.ottawacaregiver.com